Survive NICU
No matter what the circumstances or what your experience is, everyone has the same objective when their baby is born premature: Survive NICU life.
Not only are you scared for your baby, but your whole life changes and your priorities shift. While not everyone may be able to be there all day, every day, you do your best to be with your baby as much as possible. Some people still need to work or have other children to care for at home. Splitting your time between two worlds takes a toll on everyone involved.

Today’s family knows all about what it takes to survive NICU life. Giselle, a micro preemie mom, not only shares the story of her sweet baby, but offers some really great advice on how she made it through NICU life. I wish I had some of her advice before my experience!
Now, please meet Lucia, as told by her mom, Giselle.
Lucia Wren
1. Tell us about your baby.
My daughter’s name is Lucia Wren. She was born at 25 weeks and 3 days, weighing 1 pound and 7 oz, 12 inches long.
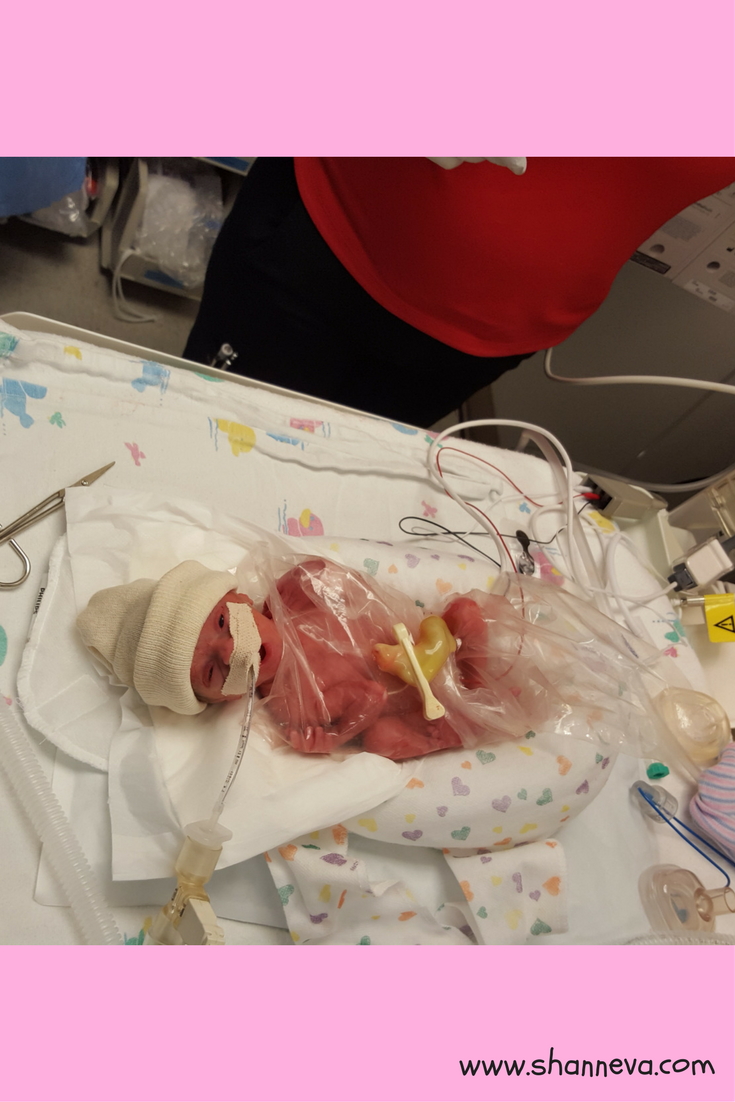
2. How long was your NICU stay?
We were in the NICU for 100 days. We are so grateful that she did amazingly well for a 25 weeker.
She had a honeymoon of 10 days, and then she started doing typical micro preemie things- Desats, Bradys, etc. Lucia had one blood transfusion and one spinal tap. She was placed in isolation twice as a precaution due to small viruses that were not serious. During her stay in isolation, she had two big apnea spells in which she had to be bagged and given breaths to start breathing again.
All her issues that she was diagnosed with during her stay -heart murmur, stage 2/3 ROP, two failed hearing tests, NG tube for feeding issues, minor chronic lung disease – were all resolved or had self-resolved by the time she was discharged and home. She was released three days before her actual due date.
3.Do you know what caused your premature birth?
This was my second pregnancy. My first pregnancy was very unexpected in that I had no idea I was pregnant till I was 23 weeks along! With that pregnancy, I delivered my son by emergency c-section at 37 weeks. When he was delivered, it was discovered that I had a bicornuate uterus (aka- heart-shaped uterus).
When I got pregnant with my daughter (9 years later), I mentioned to the doctors that I should be labeled as high risk because of my condition. Since I was at a new hospital, they told me that they did not see evidence of a BU in the scans and that I should be “fine”.
Five days before I delivered my MP, I had gone to my doctor for a scheduled exam and I reported that I had decreased fetal movement, cramping in my lower back, a pain in the right side of my stomach that would go away and come back, and weird discharge. I was told that what I was feeling was normal and that the discharge could be a yeast infection. I was given a pill to take for the “yeast infection” and sent home.
During the next five days, I continued to feel the same symptoms that I had reported to my doctor. Since I was sent away feeling like I was being too anxious, I just went about my regular routine of working out and lifting weights (which I had been cleared for since the early weeks of my pregnancy).
On the evening of the 25th of January, I had returned from my lifting class and noticed that I had a lot of blood. A lot. I called the advice nurse and was told to do to go to Labor and Delivery Triage department of the hospital. When I arrived they immediately checked for a heartbeat (which was at 145). After many scans and exams, they gave me steroids and called an ambulance so that they could send me to a hospital that could take a 25 weeker.
As soon as I got to the ER, they were hopeful that they could keep her in there longer, but minutes later things took a turn. My vitals and her vitals were going down and fast. They had no choice but to take that minute via c-section. The doctors told me that when they got to her they saw that she had zero measurable fluid, her umbilical cord was starting to detach, and there was a sever infection in my uterus.
It was determined that because the egg had implanted in the smaller horn of my uterus, my membranes ruptured (but not completely) and I was leaking amniotic fluid the whole time. From there, I developed an infection that luckily did not affect my daughter. When she was born, she was immediately given antibiotics, but had tested negative for any infection.
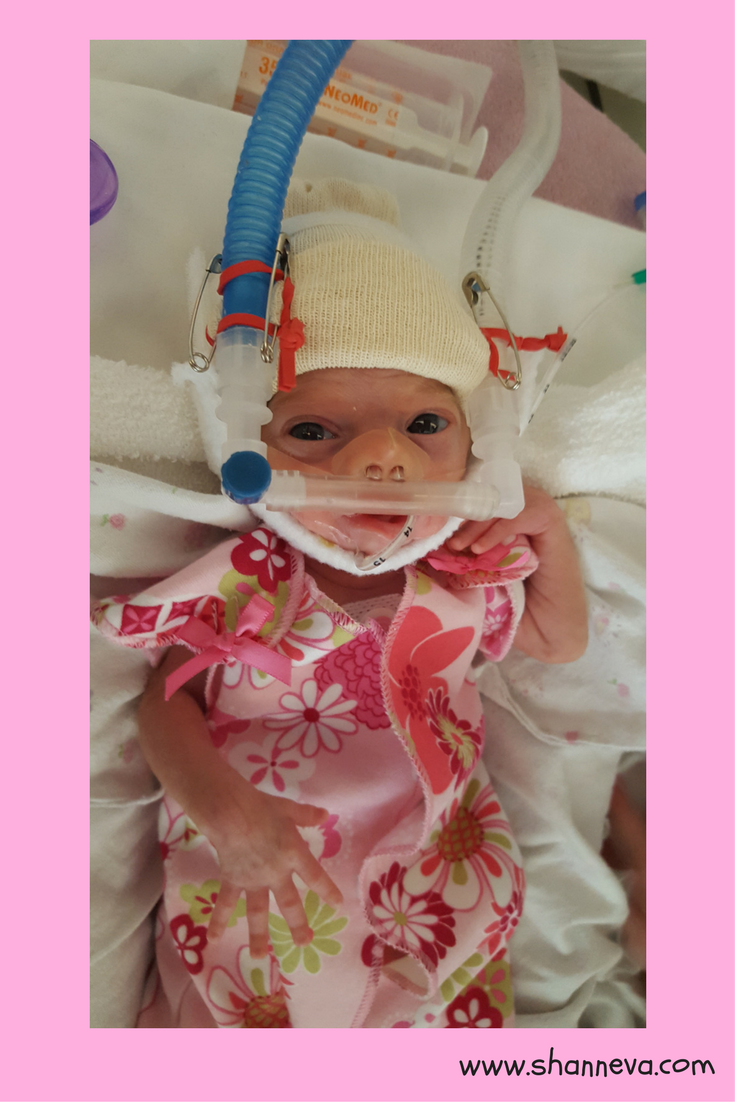
4.How are you and your baby doing now?
My MP is now 13 months old. She is a completely happy and healthy little girl. Lucia is very petite (as of right now 15 lbs and 25 inches long) and wearing 9 month clothing. She was recently taken off all her acid reflux meds and doing well in that department. Lucia has reached all the milestones for her adjusted age- crawling, cruising, clapping, playing peek-a-boo, says “mom” and “dadda”, eating solids and on whole milk. She recently had ear tube placement surgery and that went really well. She loves being read to and is just now entering the stage of “stranger danger”. She is very much an anti napper, but a good nighttime sleeper. We simply adore her.
The NICU journey was the hardest on her big brother. She was born during RSV season, so the hospital was on lock-down. No one under 12 years old was allowed to come into the NICU. I tried very hard to keep him informed as to her progress. On the days that I could remember, I would try to bring home something from the NICU for him. Whether it was a preemie diaper, measurement paper, a paci, snoodle, even a feeding tube. I just wanted him to have something tangible that he could hold. He wanted to see her so bad and it was very hard for him to know that everyday I was going to see her and he could not.

My family was fortunate enough to be in a position where I was able to take the time off and be with Lucia in the NICU. I am a teacher, so I automatically had the summer she came home off. From 8 am to 4 pm, I would go to the NICU. I pumped the whole time she was there and stopped when she came home. It was too difficult for me to get into the swing of exclusively pumping with a newborn at home. We eventually supplemented with formula, and I stopped pumping. I was okay with that since I was able to produce what she needed while in the NICU.

5. What advice would you give to a new preemie family?
Be still and don’t flail
When I was 5 years old, the last thing I had to master in swim lessons before going up a level was floating on my back. For some reason this was very hard. Every time the instructor put me on my back, I would flail my arms and totally struggle. Finally, my swim instructor just said, “BE STILL. Let the water do it’s job.” That is what you need to remember in the NICU. Things are unpredictable and scary, but if you are just “still” and let the doctors, nurses, and your preemie do their thing, it will be fine, I promise.
This is your NEW JOB! The first few days are hard but I promise, it will get better. It is really hard to see it, but it will.
When I was still recovering in the hospital and went down to the NICU to see her, I felt so overwhelmed. Every time I entered the doors of the NICU, I felt like I was suffocating. I did not want to be there, and I definitely did not want my baby to be there. At one point, I think I just went into survival mode. I just had to change my thinking. This is where she was and this is where I needed to be. I know it is going to sound cold, but I had to treat it like a new job. I had to develop a new routine to create some stability in a situation that was anything but. So I did. I show up everyday, pump, hold her, do her cares, eat, and repeat. For 100 days this was my job, and I just kept my eye on the prize- TAKING HER HOME.
Choose some primary nurses
Shortly into her stay we were told that you could ask nurses to be your primaries for your baby. This means that anytime a nurse is on duty, they will be assigned to your baby. I will say that it is a little nerve-raking to “ask” a nurse to be your baby’s primary. I felt like I was in high school asking someone out again. The very first nurse I asked declined and that itself is hard to handle. Some nurses don’t like to be primaries or want to get too attached to babies, and that is understandable. Don’t take it personally and just ask another. One of the primary nurses that we had for our daughter is still a close friend of mine today.
Talk to other parents in the NICU
Whenever I would go out and eat my lunch in the waiting area, I would try to talk to anyone and everyone that I thought was a parent in there too. There were several mothers that came up and helped me out tremendously in those first few days. They knew exactly what I was feeling and always knew exactly what I needed to hear. Because of these beautiful mothers, I made it a point to try to comfort other mothers during those first days of their journey. A few words go a long way. Say hi, offer a shoulder, ask them about their day. You get to know people and it is nice to have someone to talk to who is going through the same thing. I still keep in touch with various families that I have met in the NICU and it is so nice to see their preemies growing and thriving as well.
Take time for you
Like I said before, I would only go to the NICU from 8 to 4. My husband to try to make the drive in after work when he could, but we still went back to our regular lives. I had a nine-year old that I still needed to be home for and a household to take care of. I found that getting back into my typical routine “after work” helped a lot. Once I was cleared, I began attending my regular evening gym classes. I would call the NICU every night before I went to bed and then every morning before I headed out on the road. Again, all a part of my new routine.
Have a baby shower!
Before my daughter arrived a date for a baby shower was already in place. People still asked me if I wanted one, and my first thought was NO! But after talking to friends and family, I came to the realization that just because she was early does not mean I can’t celebrate her. We choose to have it on the originally scheduled date, and it was really nice to see everyone and open all the cute and wonderful things that she would get to use when she was finally home.

Feel the guilt and then let it go
You are going to feel guilty, there is no way around it. You feel guilty that your baby is in there; guilty that you may have done something wrong; guilty every moment you are not there; guilty that you feel guilt when your baby is doing well and others are not; guilty about everything. My advise to you is FEEL IT. Have yourself a pity party and then LET THAT STUFF GO. You feeling guilt does not help anyone- not you, not your baby, not your SO, no one.
Your body did not fail you, it did its job. I used to feel like my body failed my baby some how. In reality, my body did it’s job and basically saved my baby. My body knew something was wrong and got her out of there. I realize this is hard for people to accept and not every situation involved in preterm delivery is the same, but for me and my situation, I know that my body did what it was created to do. It knew that I had an infection, knew that my baby was in danger and got her out of there.
Not every journey is the same. People are different, babies are different, doctors are different, and hospitals are different. Keep that in mind when you are hearing or reading about other people’s stories. People process things differently. My course of grieving and the way I dealt with everything is not the same as others, but I do know that there are people out there that can relate. I feel that part of my mind shut off from the first signs that told me she was coming early.
Normally, I am a very anxious person, but for some reason I remained very calm through her delivery and after (I did have my breakdown moments). Basically, I just feel like the journey in the NICU is just a surreal memory at this point. I used to feel bad that I did not feel the same as other mothers when would read about their stories and their emotional struggles after the NICU. Whenever I feel this way, I have to remember that this is how I deal with it. Not everyone will deal with it the same. Respect that. Accept that.
FB Support Groups
There are a ton of support groups on FB for everything. It is a great place to read stories and get advice. If you are on FB, I highly recommend that you find one that fits your situation. If you are not on FB, ask the social worker in your NICU about other groups that they may know about.
Thank you so much to Giselle for sharing Lucia and their story with us. Her advice on how to survive NICU life is amazing, and I think it will help anyone who is beginning their journey.
Please leave any supportive comments or questions for Giselle and Lucia below.


She is so precious! What a tough time but I am so glad she is thriving!
What an amazing adorable baby! Thank you for sharing your story, it will help so many other parents in similar situations. Your advice to be still and not flail is valuable advice for so many of us.
She is adorable, I know this post will help other mothers in the same boat. Thank you for sharing your story.
This is such amazing advice for NICU moms! I think developing that routine would help so, so much. Allowing everyone to do their job–so important but must be so hard when you’re under that kind of stress.
These tiny ones are so brave! I love reading their stories and the wisdom these parents share with other NICU parents!
She is growing into such a beautiful little girl! I had no idea about asking for a primary nurse in a NICU…reminds me of a primary caregiver in childcare. Makes perfect sense. What a great tip!
Aw, your daughter is so so adorable!! It’s wonderful you are sharing your story.
I am so glad to hear she is doing well! I couldn’t imagine what these parents go through.
Omg what a cutie!!!!!!! So glad to see her doing well!!!!