Miracles
Whether you believe in miracles or not, today’s Micro Preemie Monday story is pretty amazing.
Coincidentally, today’s story features a baby named Sophia, who battled IUGR, just as another Sophia did, who we met two weeks ago. While their stories are uniquely their own, those similarities are very important. I know I feel a connection when I can find details that are the same as what I went through in my premature birth. It’s my hope that by sharing these stories, others feel the same way, and can feel comforted.
Miracles can and do happen.
Please meet Sophia, as told by her mom Cassy.
Sophia
1.Please tell us about your baby.
Sophia was born at 25 weeks at 6 days. She weighed 1 pound and 1 ounce and was 11.5 inches long. She was born at 16:17 on August 18, 2014. It was one day after our first wedding anniversary.
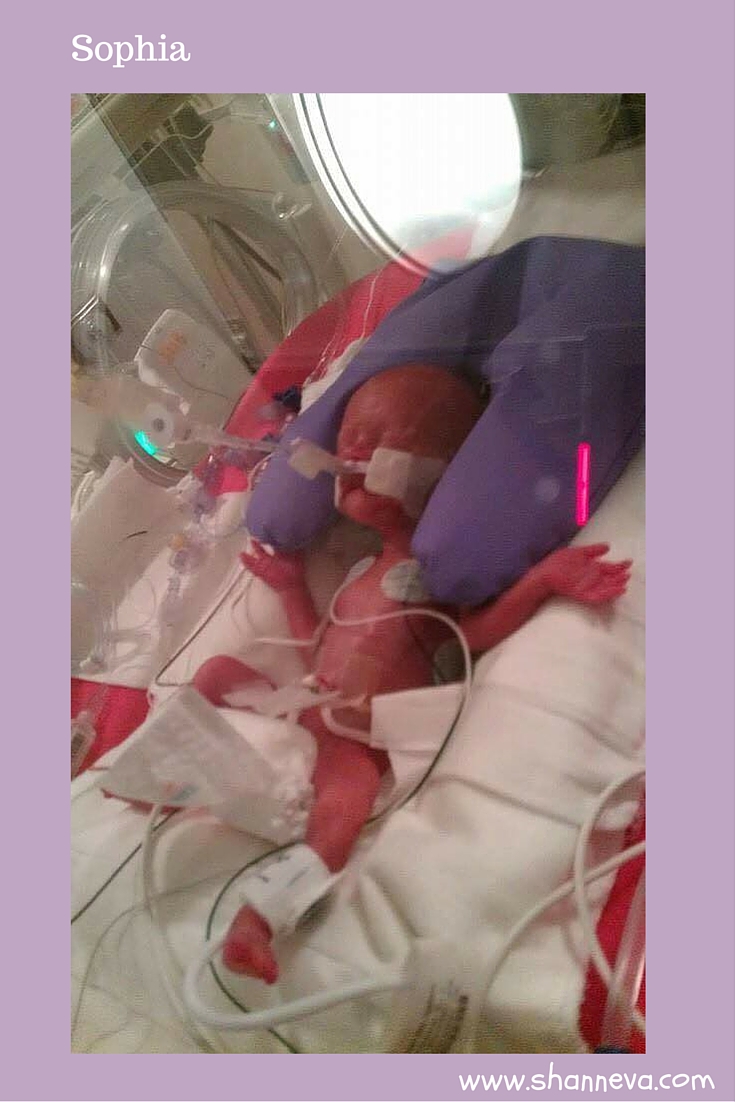
Premature Birth
2. Do you know what caused your premature birth?
We found out at 20 weeks we had IUGR, she was a week behind. At 24 weeks, she was 2 weeks behind and the doctor noticed she had Absent End Diastolic Flow (there was a pause in the blood flow through the umbilical cord after each heartbeat). The high risk specialist told us we would be having her in 3-4 weeks. I received Betamethasone shots to help her lungs develop. At 25 weeks, she was 2.5 weeks behind and now she had Reversed End Diastolic Flow (the blood flow was backing up in the umbilical cord after each heart beat). They did a NST to check her heart rate to see if she was stable enough for us to travel 2 hours to the children’s hospital. If not, they would deliver her here, try to save her, and fly her there.
Luckily, we were able to go up there. After waiting for almost 2 hours in registration, we got into our room in the anti-partum unit. I was hooked up to a monitor for her, as well as IVs for fluid and to lower my stroke level blood pressure. A doctor from the children’s hospital came in and told us that at her size, she had a 50% chance of survival, and if she did survive, she had a 50% of being a vegetable. He told us that she would more than likely never open her eyes, breathe on her own, walk, talk, or anything.
We told the doctors that we believed in disability over death, and that they were to take every possible measure to save her life. After 6 days of monitoring, Sophia started to have Bradycardia episodes and drop her heart rate down into the 30s-40s. It was putting too much strain on her heart. We had just 3 hours until the OR would be ready, and then they were taking her. Our families were 2 hours away and barely made it before they took me back. I had a classical c-section where they cut horizontally through my abdomen and vertically through my uterus. I couldn’t go through labor because Sophia wouldn’t survive. A normal c-section was too dangerous for her as well.
The Miracles Begin
3.Tell us about your NICU experience.
Her first miracle was that she was still completely encased in her amniotic sac when she was born, which is very rare.
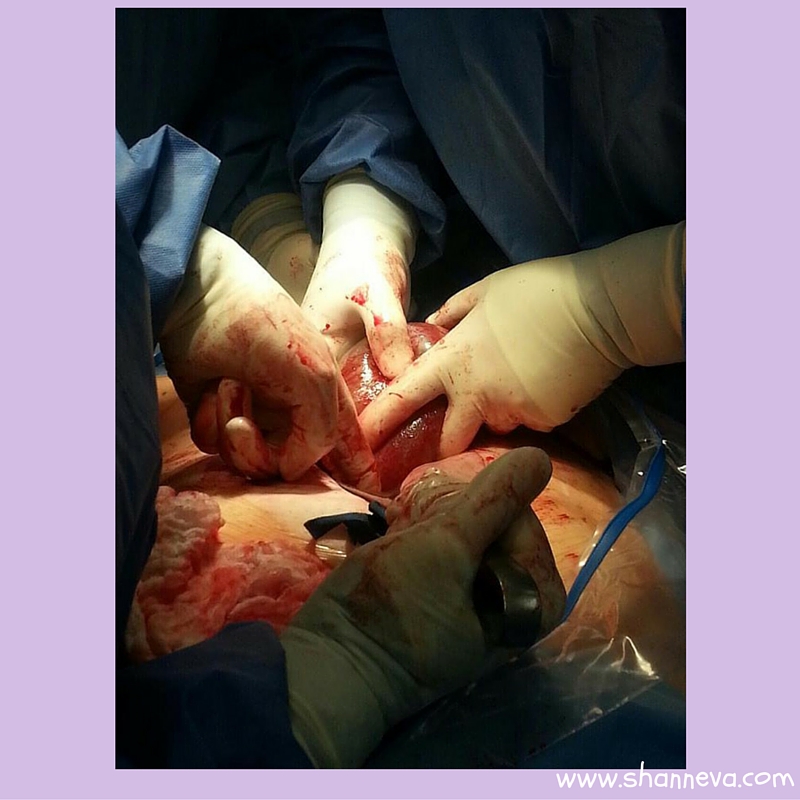
The second miracle was that she was taking tiny breaths all on her own, but they were not strong enough to support her. She was immediately intubated. Her APGAR scores were 1, 5, 7. She was with us at my hospital for about an hour and a half. I know I saw her in the OR and in recovery from pictures, but I do not remember it at all. She was transferred 15 minutes away to the children’s hospital.
The respiratory therapist on the transport said Sophia was the smallest baby she’d ever taken care of. It was 24 hours before I was able to go “on pass” to see my daughter. I don’t remember seeing her that day either. I was able to be gone from my hospital for four hours each day. I was there for 5 more days. It killed me not being able to see my daughter. I was under heavy medications and didn’t (and still do not) know everything that happened when I wasn’t there. My family has told me they almost lost her several times and that my husband had several breakdowns while he was there with her. They wouldn’t tell me so I would stay calm and they won’t talk about it now because it’s the past and it doesn’t matter.
Her doctor was the NICU director of 34 years, and he said she was the sickest baby he’d ever seen.
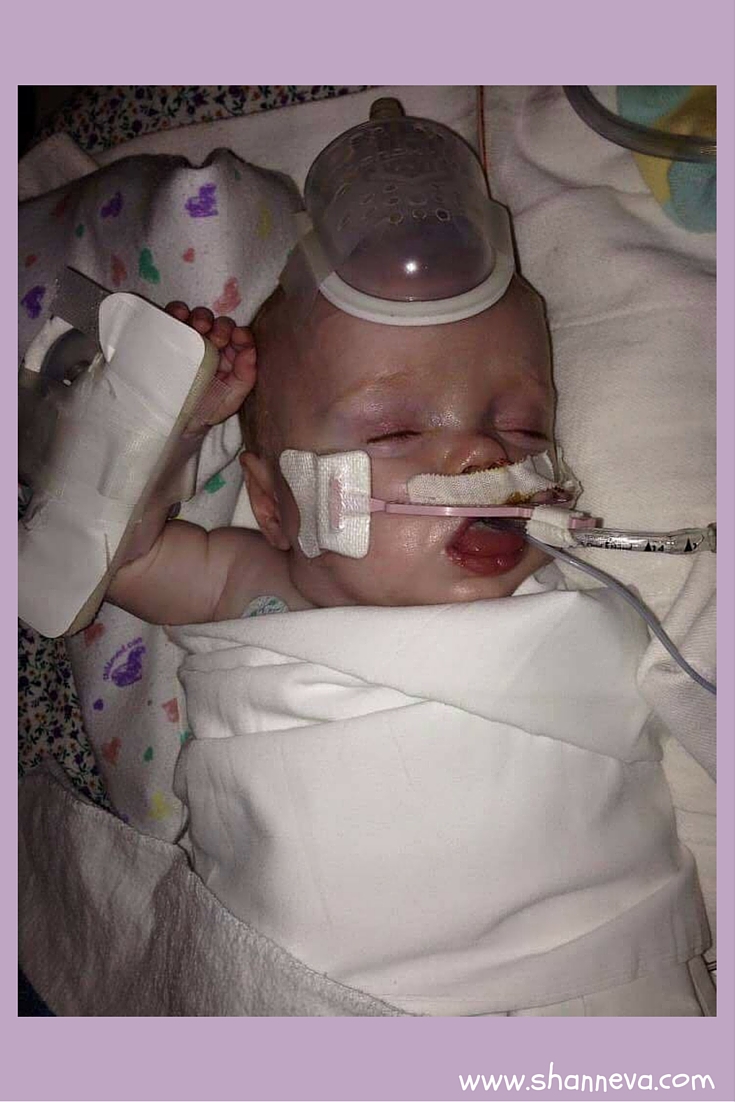
Her due date came and went, and we were told it would still be several months until she could come home. I was not working at the time and I stayed with her 99% of the time, while my husband was 110 miles away working and taking care of our pets. This broke our hearts because we longed to be a family of three at home. A month later, I was able to talk to our primary neonatologists and they decided that our NICU at home (where my husband works) was capable of providing her the c-pap that was keeping her from discharge.
We transferred her to his hospital on his birthday (he didn’t know until the night before when he came up to visit!).
Seven weeks later, Sophia started to get sick. She had went to high flow cannula the week before. We had to go up on her oxygen, and she was very lethargic. All her labs had come back clear, but an echo showed that she had pulmonary hypertension. A blizzard was on the way, so we decided to transfer her back to the children’s hospital as a precaution. If we waited, we may not have been able to get her up there if necessary.
The transport team arrived 2 hours later. They put her back on c-pap at a PEEP (Positive End-Expiratory Pressure) of 5. By the time they arrived at the children’s hospital, she was on a PEEP of 9. An hour later, she was on a PEEP of 10. She was intubated and sedated less than 12 hours after getting there. After two days of medication and maximum ventilator support, she was not breathing on her own. On her 6 month birthday, the director of the NICU said that he was very disappointed because she was not responding to any treatment, and they were running out of options.
More Miracles
He gave her 24 hours to improve, and then we would have to look at letting her go. I became numb and left the room. I don’t remember walking, but I ended up on the floor in the chapel at the foot of the cross. I fell apart begging my Lord and Savior for a miracle. Someone fetched the chaplain and when she saw my face and all I could say was, “My Sophia, my Sophia,” she cried with me. My mom knew where I had gone and came and the three of us wept and begged God for help at the foot of the cross.
I was able to hold her for the first time in 3 days, and probably the last time. I told her primary neonatologist that I would hold her for the next 2 years or as long as it took for her to get to 10 kg so that she could get a lung transplant, but I would not pull the plug on my child because I believed in miracles. Two hours later, she had X-rays done and my husband got to hold her for the last time while I went to eat. My mother was walking back and saw the NICU director running to our room asking for the parents.
I rushed in and he said that he didn’t know how, or why, or when…but her X-rays were 5 times better than the day before. He told us to keep praying to our God, and that he was going to stay the course because he believed that Sophia would survive. Eight days later, she was extubated back to c-pap. He said that Sophia had been the closest he had seen a baby be to death and come back to health with no negative effects. He later told us he had cried in his office because he didn’t know what to do.
Miracles Continued
4.How are you and Sophia doing now?

Four months later, 290 days after birth, Sophia was able to come home. She was the first baby to come home from their NICU on c-pap. Our primary neonatologist fought for two months to convince the care team that it was possible. Other than needing the pressure support, Sophia was perfectly healthy. She had previously had a PDA that self resolved, Stage 2 ROP that self resolved, an inguinal hernia that self resolved, and a PFO that self-resolved. She had no brain bleeds, which was another of the miracles.
She does have Ventricularmelegology with Hydrocephalus as well as Chiari MalformationType I. The V-H had improved to the point where no treatment has been needed and we will monitor annually. The Chiari will never improve but is luckily the more mild formation and should only cause mild headaches. She has only gained 4.5 pounds in a year. She is the classic Failure to Thrive baby. She has oral aversions to baby foods and most solid foods. We had a g-tube inserted last month. Healing has been horrible with viruses and infections, but we are hoping it will help her grow and develop. She only used the c-pap at home 24/7 for 3 weeks and at night for another 4 weeks after that. She’s been on oxygen since.
Sophia is now 22 months old (18.5 corrected). She has the peg-tube as mentioned. Hopefully we can get the g-button next month. She is 15 pounds 4 ounces and 28.5 inches tall. She wears size 6 month shirts and 3 month bottoms. She wears size 2 diapers (we wore size 1 for 13.5 months). She is walking and baking basic consonant sounds (da, ba, ga, and ma). There are some definite speech and developmental delays; however, there are other milestones she met on time or even early.
We’ve learned since day 1 Sophia does everything on her own timing. She receives speech therapy an hour a week and occupational therapy once a month. She graduated from physical therapy 6 months ago! Sophia got the OK a week ago from her primary that she can go without oxygen during the day (and her SATS have been marvelous)!
She is and always has been a very happy baby. She only fusses or cries when something is wrong. She loves running around all day and squealing, and we learned last month on vacation that she loves to swim! She’s currently snuggled up to me taking a nap, and I’m soaking it up because this moment, as well, is just that in this big miracle…a moment.

Advice
5.What advice do you have for other preemie parents?
To new Micro-preemie parents: Breathe. Remember to breathe. Us MP parents call it the NICU Tango. You’ll go back and forth a lot. Don’t get discouraged. Taking a step back allows your baby to breathe and rest so they can get stronger. They’re working hard all the time. When we workout we need to take breaks and time to recover. Living and surviving is their workout, 24/7!
Enjoy every moment and take lots of pictures. You’ll say you’ll never forget how little they were…but you will. You’ll look back and be amazed! Take lots of notes of when baby does what, and be as involved in your child’s care as much as possible! Ask lots of questions! Rest when you can and take breaks when needed. Get out of the hospital, go for a walk, go watch a movie, TAKE A NAP! You have to take care of yourself too. Your baby needs you to take care of yourself.
Use the parental support programs the NICU or hospital provides! They’ll keep you sane! It is OK to cry and ask for help!
Other MP parents are always here to listen and understand because nobody understands unless they’ve been there. People will make good-natured comments that may hurt; they don’t mean it. They just don’t understand because they don’t know. Most of the world is uneducated about the MP world. I often tell people “You’ll never truly understand what we’ve been through and why we are so careful with her until you go through it yourself, and I hope you never understand it.”

Thank you so much, Cassy, for sharing your miracles and beautiful Sophia with us. Please leave any supportive comments below.


God bless Sophia & her parents! What a heart wrenching story, but one full of God’s miracles and the power of love.
Thank you!
What a gorgeous little girl and a touching story. GOOD FOR YOU for not pulling the plug on your daughter. I’m not judging others, but I absolutely applaud your faith. God does provide miracles- and she is definitely that. God bless you!
Thank you. Before she was born we decided God was going to work miracles and that we would take disability over death. He hath provided.
Thank you so much for sharing your story. As I was reading it, I struggled not to cry – you are so strong and your strength and determination has helped Sophia! She’s a beautiful little lady!
Thank you Dana. She truly is the biggest blessing. It’s amazing to witness a miracle each day.
Miracle Baby Sophia is precious and so adorable. She is blessed to have amazing parents and Sophia is a true blessing to them as well. Amazing family memories and a big God!
Wow – I have chills reading this story. I can’t imagine what that 24 hours must have been like. I am so glad God answered your prayers and you got your miracle 🙂 What a precious gift!
What an incredibly strong family. I couldn’t imagine being in your shoes!..You are blessed.
What a fighter! This story gave me goosebumps all over! Not to take the spotlight from the amazing little girl, I was born with a congenital heart disease and at age 7 months, the doctor told my mother “to give me to the Lord” and focus instead on my younger brother. I had an open heart surgery when I was 3 years and with God’s will, I am now 46 years old 🙂
Wow what a miracle – or combination of miracles! She was so tiny, she’s done amazingly.